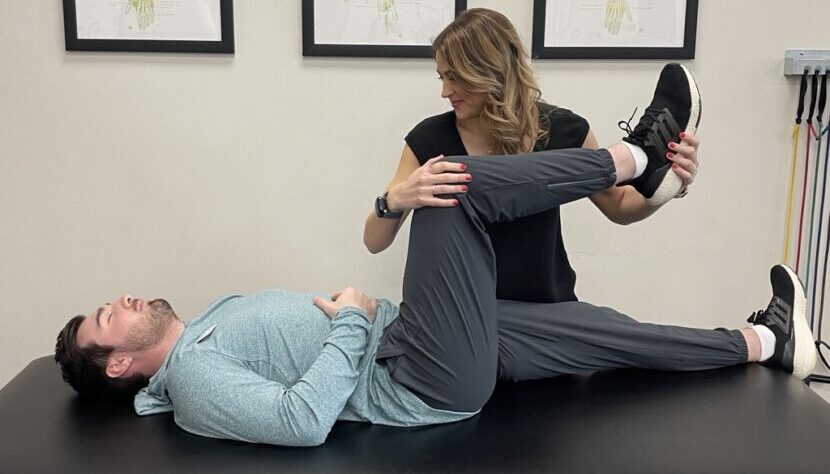
Treatment guidelines advise which therapies may help knee osteoarthritis and put off surgery – and which ones don’t.
By Emily Delzell
However you ended up with knee osteoarthritis (OA) – whether from an injury or carrying some extra weight on your joints or the genetic luck of the draw – the result is pretty much the same: pain and less ability to live an active life. But there are ways to ease discomfort and delay or avoid knee replacement surgery.
Recently published guidelines from several medical organizations offer people with knee OA and their doctors a larger toolbox of treatments – and a better breakdown of the risks and benefits.
“All people are different, both in their experience of pain and their goals, and we’ve taken a more patient-oriented approach to recommendations,” says Timothy McAlindon, MD, chief of the division of rheumatology at Tufts Medical Center in Boston and lead author of the 2014 Osteoarthritis Research Society International (OARSI) guidelines for management of knee OA. “There’s also growing concern about the toxicity of drugs, particularly for people with osteoarthritis, who often have other conditions.”
Dr. McAlindon says these concerns are weighting expert opinion in favor of non-drug treatments, and the OARSI guidelines, as well as recommendations published by the American Academy of Orthopedic Surgeons (AAOS) in 2013 and the American College of Rheumatology (ACR) in 2012, reflect this trend.
Exercise
It’s probably not a surprise that OARSI, AAOS, and ACR guidelines all heavily emphasize that exercising regularly and losing extra pounds are the best ways to get relief from knee OA pain.
“Losing excess weight and building more muscle are also the only two things that the research shows can positively affect the course of knee osteoarthritis,” says Neil Segal, MD, associate professor of orthopedics and rehabilitation and director of the Clinical Osteoarthritis Research Program at the University of Iowa in Iowa City. Other treatments target only OA symptoms, he explains.
Losing just a little weight can have big effects. Research shows that each 1-pound loss reduces the load on the knees by about four pounds. Dropping about 5 percent of body weight reduces pain and improves one’s ability to move, and losing a more significant amount – 10 percent or more – slows the disease process, according to a large trial of people with knee OA. Research published in the Journal of the American Medical Association in 2013 shows weight loss also lowers levels of the body-wide inflammation that contributes to joint damage in OA and related conditions.
Exercise not only makes dropping pounds easier, but it also can improve the pain and disability of knee OA by stopping the domino effect of inactivity leading to weakened muscles, worsening OA, increased pain and less mobility, says Amanda Nelson, MD, a rheumatologist at the Thurston Arthritis Research Center at the University of North Carolina at Chapel Hill.
Tai chi, a low-impact exercise based on slow, flowing movements, is recommended by the OARSI and ACR guidelines. It improves pain, stiffness and physical function by up to 36 percent in people with OA, according to a 2013 review of trials of the therapy.
“It’s a mind-body exercise and arthritis is a mind-body disease,” says Dr. McAlindon, who notes tai chi also lowers stress, which can influence people’s experience of pain. “It also improves lower-body strength, which is important for people with knee OA.”
Physical Therapy
A physical therapist can target your weak spots and help improve your balance, strength and joint alignment. Recent research provides more detailed guidance for therapists treating people with knee OA, Dr. McAlindon notes.
The ACR and AAOS guidelines recommend exercise supervised by a physical therapist. The AAOS expert panel notes that most of the studies that showed strong evidence for exercise benefiting knee OA involved programs led by these specialists, who can also advise on biomechanical devices such as braces and orthoses.
Anil Bhave, a physical therapist and director of the Wasserman Gait Laboratory at the Rubin Institute for Advanced Orthopedics in Baltimore, prescribes exercises that improve strength and flexibility in the hips, hamstrings and quadriceps.
“Up to 70 percent of people with painful knee OA have weak quadriceps,” says Bhave, adding that these thigh muscles are major contributors to knee joint stability and cushioning.
Self-Management
All the guidelines and experts agree that education and self-management – building a strong understanding of how OA affects you, as well as your best therapeutic and mental strategies for coping – are among the top recommendations for coping with knee OA pain. But what is ideal self-management?
Dr. Nelson sees it as, “Learning about your disease, including what’s likely to help and what’s likely to hurt. Many people, for example, think exercise is going to hurt their joints, when it fact it will improve their condition and their pain.”
The key, says Dr. Segal, is recognizing the difference between beneficial exercise and activities that stress joints. “In knee OA, bending, stooping and kneeling increase joint damage,” he says. Rapid pivoting moves like those done in soccer or downhill skiing also can cause problems.
From Bhave’s perspective, self-management means understanding your physical limitations.
“Don’t go out and play sports on the weekend without stretching first,” he says. “Take it slow, warm up and build up. Try doubles tennis instead of singles or cross-country skiing instead of downhill, for example.”
Acupuncture
Although the AAOS guidelines recommend skipping acupuncture because there’s very little good-quality evidence that it works better than placebo,both the ACR and OARSI experts take a softer line. These guidelines stop short of endorsing the therapy, but note some trials do show a benefit and that, for certain patients, particularly those who have multiple health problems that limit treatment options, acupuncture may play a role in managing knee OA pain.
A Cochrane Database review of clinical trials of acupuncture for knee and hip OA found the therapy improved pain by about four points and physical function by about 11 points on a 20-point scale after eight weeks of treatment.
Dr. Nelson advises patients interested in acupuncture to give it a try and see if they benefit. (To find an accredited acupuncturist, ask your doctor for a recommendation or search the practitioner directory on the National Certification Commission for Acupuncture and Oriental Medicine website or the American Academy of Medical Acupuncture site.)
Spa Therapy
OARSI’s 2014 guidelines include its first-ever recommendation for balneotherapy, which can include soaking in heated mineral water, visiting mud baths or getting a water massage.
“Several studies now support water therapy for improving knee OA pain,” says Dr. McAlindon, who notes OARSI recommended it for people with OA in multiple joints and complicating conditions that leave them with limited treatment options. Studies show people with rheumatoid arthritis get similar modest benefits.
In some studies showing water therapy improved pain and stiffness, patients got treatments for more than an hour a day almost daily for three weeks, so soaking in your home tub for 10 minutes isn’t likely to lead to any lasting improvements.
Although balneotherapy is more common in Europe, where it’s often prescribed for OA pain, your doctor may be able to suggest facilities that provide similar therapies.
Joint Alignment
Problems with biomechanics – how the spine, hips, knees and feet line up to work together – worsen the pain of knee osteoarthritis (OA) and damage affected joints, says Bhave.
“Most people with knee OA have some kind of malalignment,” he says. “Being overweight makes these problems worse by increasing abnormal forces through the knee.”
There are so many types of custom and off-the-shelf biomechanical devices, which include wedged insoles, various types of braces and therapeutic shoes, that studying them is tough, and evidence for their effects on knee OA is mixed. But recent guidelines from the OARSI and the ACR put them high on the list of options for people with knee OA and advise most patients (your doctor can tell you whether you’re in this group) to get a biomechanical evaluation from an appropriate specialist – usually a physical therapist.
A recent review of 25 studies of different biomechanical devices worn by people with knee OA found that knee braces and foot orthotics decreased pain, joint stiffness and the amount of pain medication they needed.
Taping the kneecap or wearing a neoprene sleeve can also adjust alignment as well as proprioception, the body’s sense of where the joint is in space, improving how the body loads the knee, says Dr. Segal. (Physical therapists are often the ones to tape a kneecap, but a patient can learn to do it.)
“Although research hasn’t proved correcting alignment can slow or stop progression of knee OA, it can reduce pain and improve people’s function, which may help them put off surgery,” he says.
What Works for You
Here’s what readers have told us works for them (based on the responses of 334 members of the Arthritis Foundation Online Panel and the Arthritis Today Reader Panel):
- Hot or cold compresses – 54 percent
- Losing weight – 42 percent
- Stretching – 36 percent
- Over-the-Counter rubs, gels or patches – 35 percent
- Walking – 32 percent
- Swimming – 28 percent
- Other exercise or physical activity – 23 percent
- Knee brace – 23 percent
- Shoe orthotic/insert – 20 percent
- Soaking in Epsom bath or hot tub – 17 percent
- Yoga – 14 percent
This article was originally published on the Arthritis Foundation Website. Click here to view it in its original form.